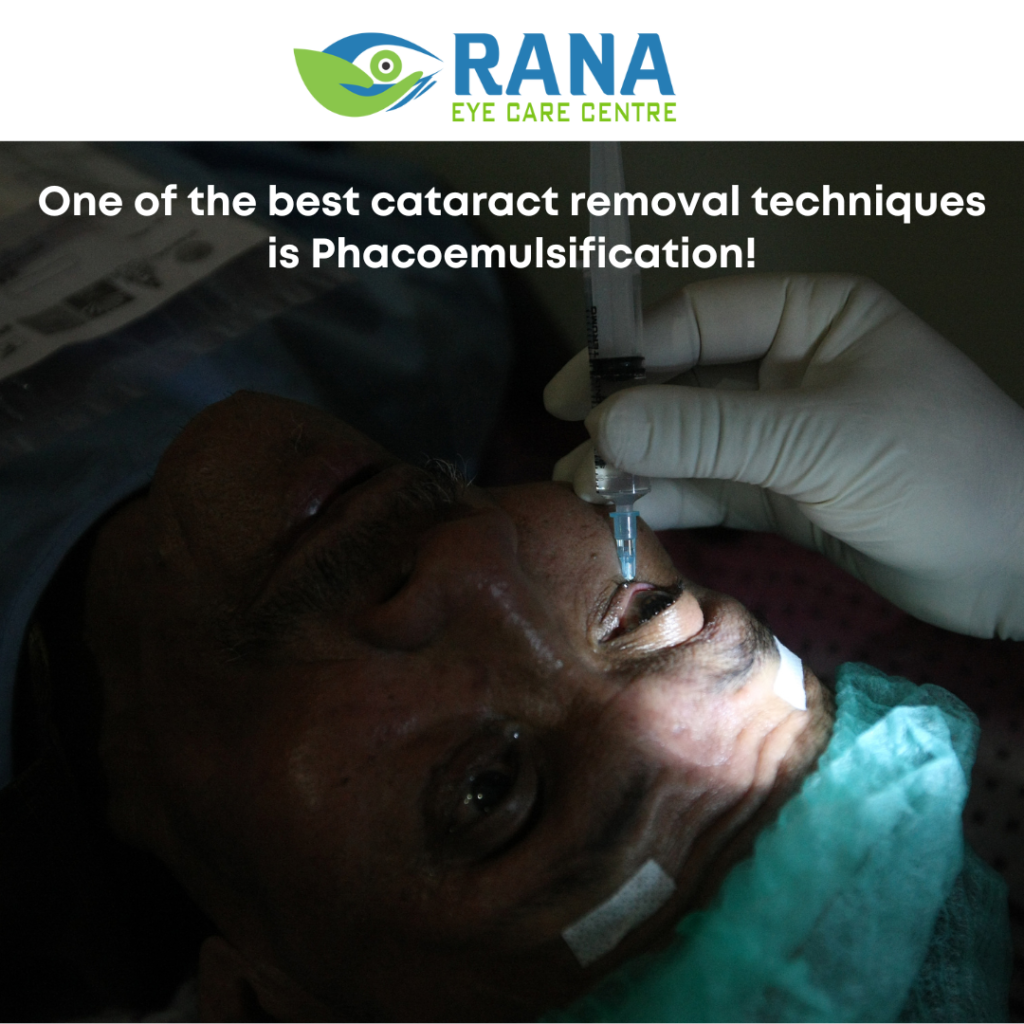
One of the Best Cataract Removal Techniques is Phacoemulsification!
Charles Kelman developed phacoemulsification, the current method for removing cataracts, in 1967. With the advent of phacoemulsification, the medical community breathed a sigh of relief, which enabled the dissolution of a cataractous lens with an incision as tiny as two to three millimeters, with perfect visual outcomes. Phacoemulsification is still the best method for eliminating cataracts, despite many advancements in recent years. Phacoemulsification cataract surgery helps restore vision in patients affected with cataracts, a clouding of the eye’s lens.
Phacoemulsification, sometimes abbreviated as “phaco,” eliminates cataracts involving microscopic incisions to break apart and remove a natural lens with cataracts. The ancient Greek term phakos, from which we get the word “lens,” is where this originates.
Why is phaco cataract surgery essential?
Cataracts are clouding of the lens of the eye, which causes vision loss and makes normal activities challenging. Surgery to remove cataracts and replace them with durable artificial lenses is the only proven method of restoring eyesight after cataract damage. If your cataract is causing blurred vision, your doctor may recommend surgery to remove your natural lens and replace it with an artificial one. Soon after completing the procedure, your vision should improve.
When is phaco eye surgery recommended?
You may require cataract surgery if you are over 40 and have any of these symptoms.
- Bilateral diplopia (dual vision in one eye)
- Lights seem to have halos or create glare;
- The vision that is unclear or distorted;
- Low visibility in the dark;
- Sensitivity to light;
- Colors fading
Cataracts can occur in people under 40. A comprehensive eye exam best determines need for phaco cataract surgery. Most eye checkups involve refraction.
What Occurs During the Phacoemulsification Process?
Before therapy, the ophthalmologist uses ultrasound or laser scanning to inspect the affected eye. Tests determine the patient’s best IOL. Phacoemulsification requires a minor corneal incision and a lens membrane hole. A small ultrasonic probe breaks apart the cloudy lens. The ultrasonic tool slashes and virtually breaks the lens material into small pieces.
After eliminating lens particles, intraocular lenses (IOLs) are placed into the lens capsule. A hollow tube introduces it through the small corneal incision. Pushing through unfolds and positions the lens. Phacoemulsification does not require hospitalization. Cataract surgery is performed under local or topical anesthetic (numbing drops inserted into the eye).
Follow-up Care for Cataracts Treated with Phaco
- Phacoemulsification may cause ocular itching and fatigue. You may tear and see poorly in solid light.
- Eye drops reduce infections. Don’t drive, bend, raise, or push on your eye.
- Your doctor may recommend sleeping with eye protection for the first week. Protecting the surgical incision location aids in eye recovery. If your eye hurts or doesn’t heal, tell your doctor.
- 4 weeks should heal your eye. 90% of Phaco cataract patients see better.
Benefits of cataract phacoemulsification
Phacoemulsification cataract surgery has several advantages:
- A smaller incision means less risk and a more straightforward procedure
- A smaller incision size reduces the amount of astigmatism that is produced
- Minimal precautions, no bandages
- There are no limits placed on regular activities
- Good eyesight returns in days.
- After a week or two, you’ll need a new set of glasses.
- An early kind of vision therapy
Why Choose us
All of today’s cutting-edge technology, surgical methods, and diagnostic services are available under one roof. We are a comprehensive eye care clinic with state-of-the-art Phaco cataract surgery facilities, staffed by the industry’s most competent, dedicated, and well-informed super-specialty specialists.



No Comments